Navigating spinal health challenges effectively
The human spine is a marvel of engineering, providing support, flexibility, and protection for the spinal cord, which is vital for transmitting nerve signals throughout the body. Maintaining spinal health is crucial for overall well-being and daily function. However, various conditions can affect the spine, leading to discomfort and reduced mobility. Among these, a herniated disc is a common challenge that can significantly impact an individual's quality of life, often causing considerable pain and limiting activity. Understanding the intricacies of this condition, from its causes to effective management strategies, is key to addressing spinal health issues comprehensively and promoting a path toward recovery and sustained wellness.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
What is a Herniated Disc and How Does it Occur?
Between each vertebra in the spine are soft, rubbery discs that act as shock absorbers, allowing for movement and preventing the bones from grinding against each other. Each disc has a tough outer ring and a soft, gel-like center. A herniated disc, sometimes called a slipped or ruptured disc, occurs when the soft inner material pushes through a tear in the outer ring. This can happen anywhere along the spine, but it is most common in the lumbar (lower back) and cervical (neck) regions. Causes often include age-related degeneration, where discs lose water content and become less flexible, or sudden injury from improper lifting, twisting movements, or trauma.
Recognizing Symptoms: Pain, Sciatica, and Nerve Discomfort
The symptoms of a herniated disc vary depending on its location and whether it is causing nerve compression. A common symptom is localized pain in the back or neck. If the herniated disc presses on a nearby nerve, symptoms can radiate to other parts of the body. For example, a lumbar herniated disc often leads to sciatica, characterized by sharp, shooting pain that travels down the leg, sometimes accompanied by numbness, tingling, or weakness. A cervical herniated disc can cause discomfort and pain that radiates into the arm or hand. These sensations are a direct result of the nerve roots being irritated or compressed by the displaced disc material.
Diagnostic Approaches for Spinal Health
Accurate diagnosis is fundamental to effective management of a herniated disc. A healthcare professional typically begins with a thorough physical examination, assessing reflexes, muscle strength, and sensation, as well as evaluating mobility and pain responses. Imaging tests are crucial for confirming the diagnosis and determining the exact location and severity of the herniation. Magnetic Resonance Imaging (MRI) is often the preferred method as it provides detailed images of soft tissues, including discs and nerve roots. Computed Tomography (CT) scans may also be used, and sometimes nerve conduction studies or electromyography are performed to assess nerve function and identify the affected nerve roots, contributing to a comprehensive understanding of spinal health.
Therapeutic Options and Recovery Pathways
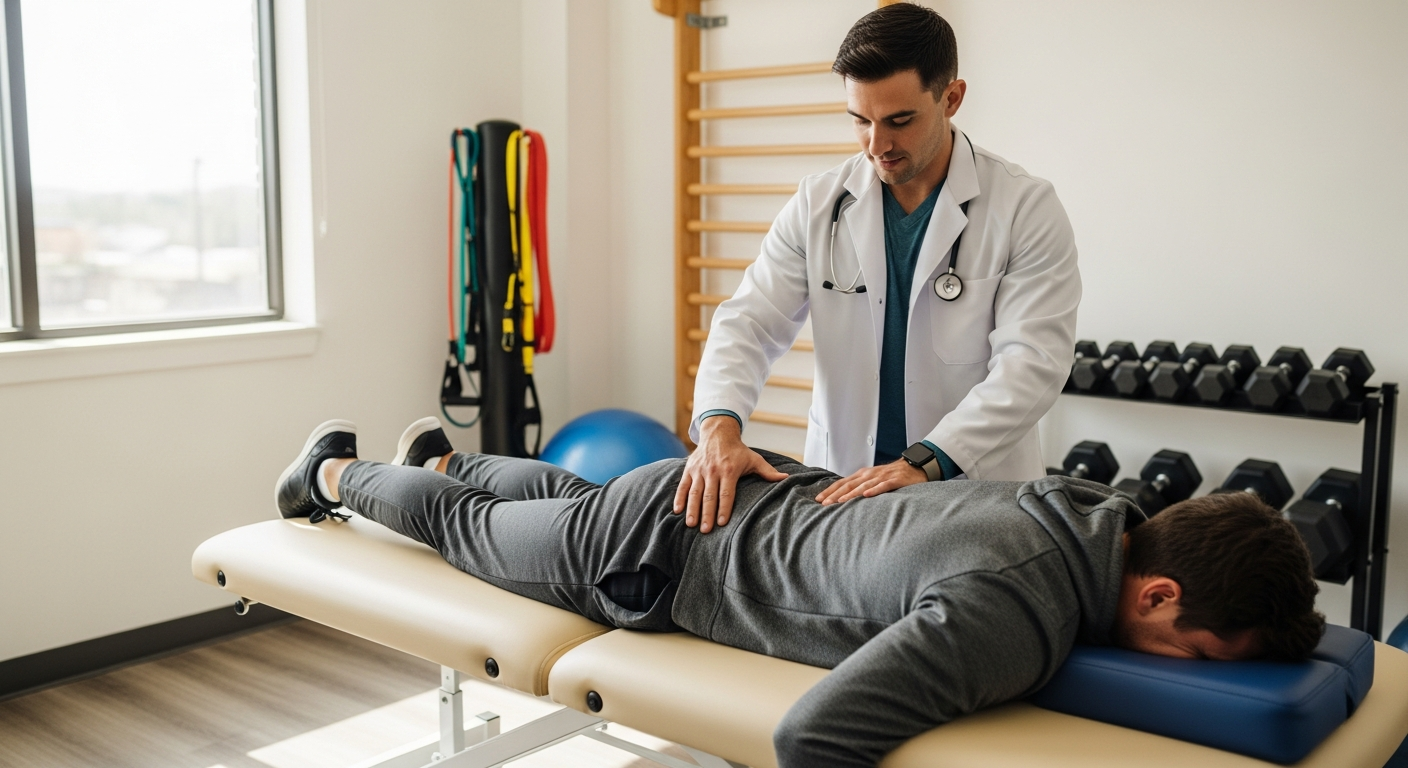
Treatment for a herniated disc typically begins with conservative methods, focusing on pain relief and promoting recovery. Non-surgical approaches often include rest, over-the-counter or prescription medications for pain and inflammation, and physical therapy. Physical therapy plays a vital role in rehabilitation, utilizing exercises to strengthen core muscles, improve flexibility, and enhance posture to support the spine. In some cases, epidural steroid injections may be administered to reduce inflammation and alleviate pain. If conservative treatments do not provide relief, or if there is progressive nerve damage or severe weakness, surgical intervention may be considered to remove the herniated portion of the disc and relieve nerve compression.
Enhancing Mobility and Posture for Long-Term Wellness
Beyond immediate treatment, adopting proactive strategies for spinal health is essential for long-term wellness and preventing future injury. Maintaining good posture is paramount, whether sitting, standing, or lifting, to minimize stress on the spinal discs. Regular, low-impact exercise, such as walking, swimming, or cycling, can help strengthen the muscles that support the spine and improve overall mobility. Incorporating stretching and flexibility exercises can also contribute to better spinal health. Ergonomic adjustments in the workplace and at home, along with body mechanics education, empower individuals to protect their back and disc integrity, supporting a healthy lifestyle and reducing the risk of recurrence.
Addressing spinal health challenges, particularly those involving a herniated disc, requires a clear understanding of the condition, its symptoms, and available treatment options. From initial diagnosis through therapy and rehabilitation, focusing on recovery and long-term wellness is key. By combining professional medical guidance with lifestyle adjustments, individuals can effectively manage pain and work towards restoring mobility and overall spinal health.